Table of Contents
A joint, or articulation, is where two bones, bone and cartilage, or bone and teeth meet. The scientific study of joints is called arthrology. Joints are classified structurally and functionally. The structural classification is based on the presence of a synovial cavity and the type of connective tissue binding the bones. There are three structural types: fibrous joints (held together by dense connective tissue), cartilaginous joints (joined by cartilage), and synovial joints (with a synovial cavity and articular capsule).
Structure of Synovial Joints
Synovial joints are characterized by the presence of a specific region known as the synovial cavity or joint cavity, situated between the articulating bones. This synovial cavity plays a pivotal role in allowing substantial mobility within the joint, leading to the classification of synovial joints as functionally “freely movable” or diarthrosis.
Within synovial joints, the surfaces of the involved bones are enveloped by a layer of hyaline cartilage referred to as articular cartilage. Articular cartilage does not bind the bones together; instead, it primarily serves to reduce friction between the bones during motion and absorb shocks generated within the joint.
The articular capsule serves to enclose the synovial cavity and connect the articulating bones. It consists of two distinct layers: an outer fibrous membrane and an inner synovial membrane.
- The outer fibrous membrane is primarily composed of dense irregular connective tissue, predominantly comprising collagen fibers. This membrane attaches to the periosteum of the articulating bones and continues the periosteum between these bones. The fibrous membrane exhibits flexibility, allowing for substantial joint movement, and possesses remarkable tensile strength, which helps prevent bone dislocation (the displacement of a bone from its joint). Some fibrous membranes have collagen fibers arranged in parallel bundles of dense regular connective tissue, known as ligaments. Ligaments play a crucial role in holding bones together within synovial joints, and they often have specific names to identify their location and function.
- The inner layer of the articular capsule, known as the synovial membrane, is primarily composed of areolar connective tissue with elastic fibers. In many synovial joints, this membrane contains accumulations of adipose tissue, referred to as articular fat pads. For example, the knee joint features the infrapatellar fat pad.
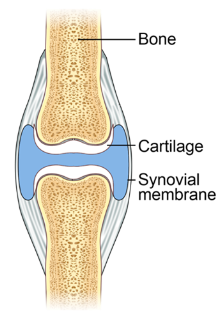
Synovial fluid, often likened to uncooked egg white in appearance and consistency, plays a crucial role in the function of synovial joints. It is secreted by the synovial membrane and comprises two main components: hyaluronic acid produced by synovial cells and interstitial fluid filtered from blood plasma. This fluid forms a thin layer over the surfaces within the articular capsule of a joint.
The functions of synovial fluid are diverse and essential. These include:
- Reducing Friction: By lubricating the joint surfaces, synovial fluid minimizes friction during joint movement, ensuring smooth articulation.
- Absorbing Shocks: It acts as a shock absorber, cushioning the joint against mechanical stresses and impacts.
- Supplying Nutrients: Synovial fluid delivers oxygen and nutrients to the chondrocytes within the articular cartilage. This is particularly significant because cartilage is avascular and lacks its own blood supply.
- Waste Removal: It helps remove carbon dioxide and metabolic waste products from chondrocytes, supporting their metabolic processes.
- Immune and Cleaning Functions: The fluid contains phagocytic cells that play a role in removing microbes and debris generated by normal joint wear and tear.
Types of Synovial Joints
Synovial joints, while sharing common characteristics, exhibit diverse shapes of articulating surfaces, allowing for a wide range of movements. They can be classified into six main categories based on the type of movement they permit:
Plane Joints (Planar or Planar Joints)
In-plane joints, the articulating surfaces of bones are flat or slightly curved. These joints primarily enable back-and-forth and side-to-side movements between the flat surfaces of bones. They may also involve rotation. Many plane joints are biaxial, allowing movement in two axes, and some are triaxial, permitting movement in three axes. Examples include the intercarpal joints (wrist), intertarsal joints (ankle), sternoclavicular joints (between the sternum and clavicle), and acromioclavicular joints (between the scapula and clavicle).
Hinge Joints (Ginglymus Joints)
Hinge joints are characterized by the convex surface of one bone fitting into the concave surface of another bone. These joints produce an angular motion, resembling the opening and closing of a hinged door. Typically, one bone remains stationary while the other moves around an axis. Hinge joints are uniaxial, allowing motion around a single axis. They permit only two types of movement: flexion (bending) and extension (straightening). Examples include the knee (a modified hinge joint), elbow, ankle, and interphalangeal joints (found between the phalanges of the fingers and toes).
Pivot Joints (Trochoid Joints)
Pivot joints involve the rounded or pointed surface of one bone articulating with a ring formed partially by another bone and partially by a ligament. These joints are uniaxial, allowing rotation solely around their longitudinal axis. Examples include the atlantoaxial joint, where the atlas rotates around the axis, allowing head movement from side to side (as in shaking your head “no”), and the radioulnar joints, enabling the palms to turn anteriorly and posteriorly as the head of the radius pivots within the radial notch of the ulna.
Condyloid Joints (Ellipsoidal Joints)
Condyloid joints are characterized by the convex oval-shaped projection of one bone fitting into the oval-shaped depression of another bone. These joints are biaxial, allowing movement around two axes: flexion-extension and abduction-adduction. They also permit limited circumduction. Examples of condyloid joints include the radiocarpal joint (wrist) and metacarpophalangeal joints (between the metacarpal bones and proximal phalanges) of the second through fifth digits.
Saddle Joints (Sellar Joints)
In saddle joints, one bone’s articular surface is saddle-shaped, and the other bone’s surface fits into it like a rider sitting on a saddle. These joints exhibit biaxial movement, allowing flexion extension and abduction-adduction, along with limited circumduction. An example is the carpometacarpal joint between the trapezium of the carpus and the metacarpal of the thumb.
Ball-and-Socket Joints (Spheroid Joints)
Ball-and-socket joints consist of a ball-like surface of one bone fitting into a cup-like depression of another bone. These joints are triaxial (multiaxial), permitting movement in three axes: flexion-extension, abduction-adduction, and rotation. Prominent examples include the shoulder joint, where the head of the humerus fits into the glenoid cavity of the scapula, and the hip joint, where the head of the femur fits into the acetabulum of the hip bone.
Factors Affecting Synovial Joints
Six factors influence the type of movement and range of motion possible at synovial joints:
- Bone structure: The shape of the articulating bones determines how closely they can fit together, affecting the range of motion. Some bones have complementary shapes that allow rotational movement.
- Ligament strength and tension: Ligaments can be tense or taut in specific positions, restricting the range of motion and guiding bone movement. Muscle tension reinforces ligament restraint.
- Muscle arrangement and tension: Muscle tension further restricts joint movement. Muscles can limit joint mobility, and their tension affects the range of motion.
- Contact of soft tissues: The contact of one body surface with another may limit joint mobility, such as when the forearm meets the biceps muscle during elbow flexion.
- Hormones: Hormones like relaxin can affect joint flexibility. For example, relaxin increases the flexibility of certain joint tissues, facilitating childbirth.
- Disuse: Joints that are immobilized for extended periods may experience a limited range of motion when movement is resumed. Disuse can lead to decreased synovial fluid, reduced ligament and tendon flexibility, and muscle atrophy.
Summary
Joints, also known as articulations, where bones, cartilage, or teeth meet, are studied in the field of arthrology. They are structurally classified into fibrous joints, cartilaginous joints, and synovial joints based on the presence of a synovial cavity and the type of connective tissue binding the bones. Synovial joints, characterized by a synovial cavity, are crucial for mobility and feature articular cartilage to reduce friction and an articular capsule comprising a fibrous outer layer and a synovial inner layer. Synovial fluid within the joint performs functions such as lubrication, shock absorption, nutrient supply, waste removal, and immune defense. These joints are categorized into six types based on their movement capabilities: plane, hinge, pivot, condyloid, saddle, and ball-and-socket joints. The range of motion in synovial joints is influenced by factors including bone structure, ligament strength, muscle arrangement, soft tissue contact, hormones, and disuse, making them vital components of the musculoskeletal system.
FAQs on Synovial Joints
What is the study of joints called, and how are joints classified?
The scientific study of joints is called arthrology, and joints are classified structurally into fibrous joints, cartilaginous joints, and synovial joints based on the presence of a synovial cavity and the type of connective tissue binding the bones.
What distinguishes synovial joints from other types of joints?
Synovial joints are characterized by the presence of a synovial cavity, articular cartilage to reduce friction, and an articular capsule comprising a fibrous outer layer and a synovial inner layer. These features allow for substantial mobility, classifying synovial joints as 'freely movable' or diarthroses.
What is the role of articular cartilage in synovial joints?
Articular cartilage, found on the surfaces of the bones within synovial joints, primarily reduces friction during joint movement and absorbs shocks generated within the joint.
What are the components of the articular capsule in synovial joints, and what functions do they serve?
The articular capsule consists of an outer fibrous membrane composed of dense irregular connective tissue, which provides flexibility and prevents bone dislocation, and an inner synovial membrane made of areolar connective tissue. The synovial membrane produces synovial fluid, which lubricates the joint, absorbs shocks, supplies nutrients to cartilage, removes waste products, and performs immune functions.
How are synovial joints classified based on their movement capabilities?
Synovial joints can be classified into six categories: plane joints, hinge joints, pivot joints, condyloid joints, saddle joints, and ball-and-socket joints. Each type permits specific types of movement, ranging from simple back-and-forth motion to multidirectional rotation.
What factors influence the range of motion in synovial joints?
Several factors affect the range of motion in synovial joints, including bone structure, ligament strength and tension, muscle arrangement and tension, contact of soft tissues, hormones, and disuse. These factors collectively determine the joint's flexibility and mobility.
How does synovial fluid contribute to joint function?
Synovial fluid reduces friction, absorbs shocks, delivers nutrients to cartilage, removes waste products, and supports immune functions within synovial joints, ensuring their smooth and efficient operation.
Can hormones affect joint flexibility, and if so, how?
Yes, hormones like relaxin can influence joint flexibility. For example, relaxin increases the flexibility of certain joint tissues, which is particularly significant in facilitating childbirth.
What role do ligaments play in synovial joints?
Ligaments are dense connective tissue structures that hold bones together within synovial joints. They can be taut or tense in specific positions, restricting the range of motion and guiding bone movement. Muscle tension can reinforce ligament restraint.
How does disuse affect synovial joints, and what are the consequences of prolonged immobilization?
Joints that are immobilised for extended periods due to disuse can experience limited range of motion when movement is resumed. Prolonged disuse can lead to decreased synovial fluid, reduced ligament and tendon flexibility, and muscle atrophy, impacting joint health and function.








